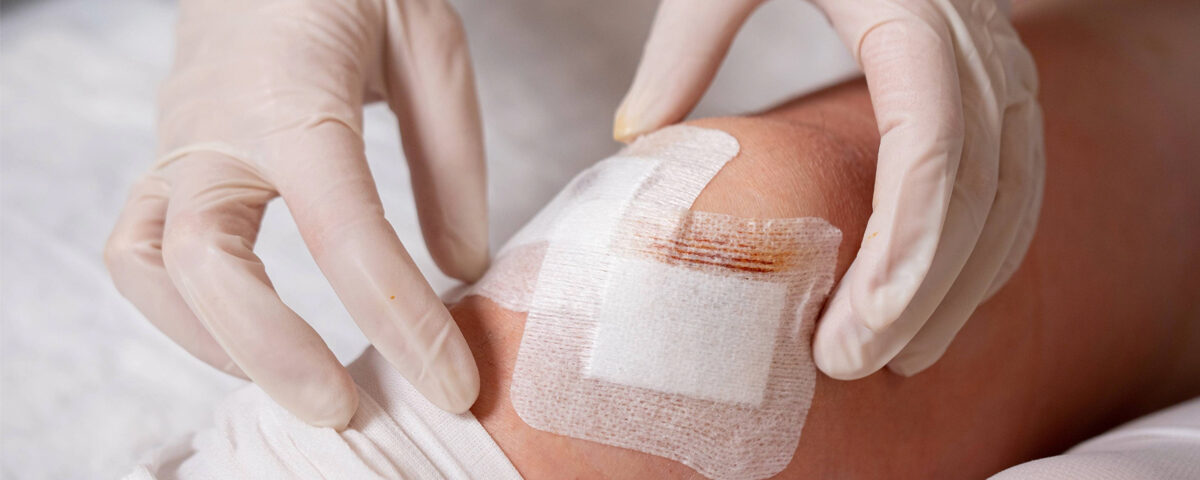
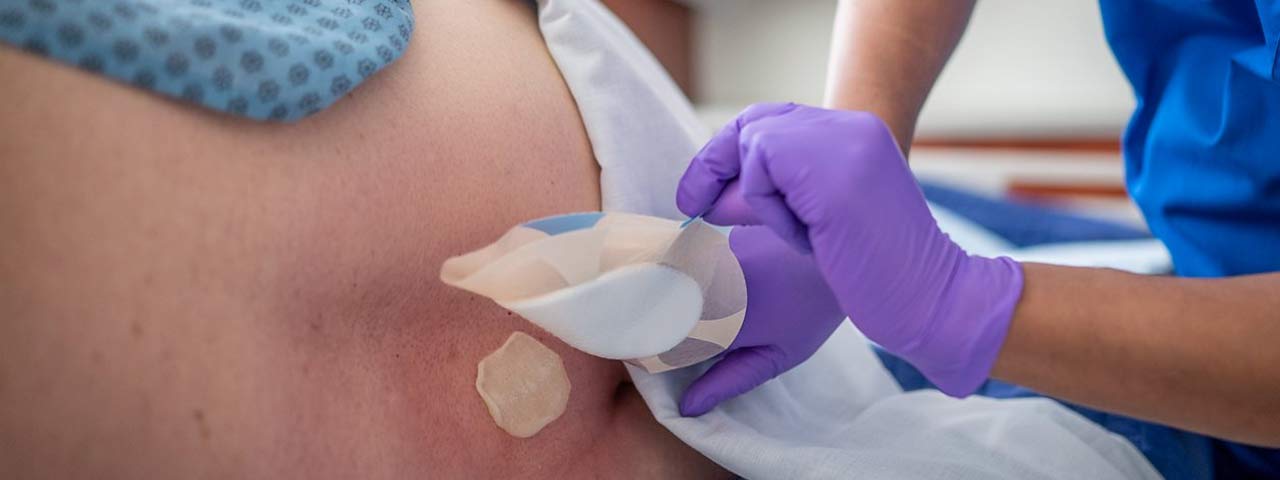
Bedsore Dressing involves the management and treatment of pressure ulcers (commonly known as bedsores) to promote healing, prevent infection, and alleviate discomfort. Bedsores typically occur in immobilized patients and require meticulous care tailored to the wound’s stage and condition.
Stages of Bedsores and Their Dressing Needs:
- Stage 1: Skin is intact but red and may feel warm or tender.
- Dressing: Protective barrier creams, hydrocolloid, or transparent film dressings to reduce friction and provide moisture.
- Stage 2: Partial-thickness skin loss with exposed dermis; may appear as a blister or shallow open wound.
- Dressing: Hydrogel, foam dressings, or hydrocolloid dressings to maintain a moist environment and support healing.
- Stage 3: Full-thickness skin loss with visible fat but no muscle, tendon, or bone exposure.
- Dressing: Alginates or foam dressings with antibacterial properties to absorb exudate and protect from infection.
- Stage 4: Full-thickness tissue loss with exposed muscle, bone, or tendons.
- Dressing: Use advanced dressings like collagen, negative pressure wound therapy (NPWT), or combination dressings to manage exudate and promote granulation.
- Unstageable: Wound covered with necrotic tissue (eschar or slough), obscuring depth.
- Dressing: Autolytic debridement dressings (e.g., hydrogel or honey-based) or enzymatic debridement agents to remove necrotic tissue.
Steps for Bedsore Dressing:
-
Preparation:
- Gather Supplies:
- Sterile gloves and dressing kit.
- Wound cleaning solution (normal saline or prescribed antiseptic).
- Appropriate dressing material (foam, hydrogel, alginate, etc.).
- Gauze pads, adhesive tape, or bandage.
- Position the Patient:
- Ensure comfort and access to the wound site.
- Minimize pressure on the affected area using pillows or special cushions.
-
Wound Cleaning:
- Wash hands and wear sterile gloves.
- Clean the wound with normal saline or an antiseptic solution to remove debris or exudate.
- Pat dry surrounding skin gently with sterile gauze.
-
Application of Dressing:
- Assess the Wound:
- Determine the wound stage and condition (exudate amount, infection signs, tissue health).
- Select Dressing:
- Use moisture-retentive dressings for dry wounds.
- Use absorptive dressings for wounds with heavy exudate.
- Apply the dressing gently over the wound, ensuring complete coverage.
- Secure the dressing with adhesive tape or bandage, avoiding excessive tension on the skin.
- Infection Control:
- For infected wounds, consider antimicrobial dressings (e.g., silver-impregnated or iodine-based) as per medical advice.
- Monitor for signs of infection: increased redness, swelling, foul odour, or purulent discharge.
General Care Tips:
-
Prevent Further Pressure:
- Reposition the patient every 2 hours to reduce pressure on bony areas.
- Use pressure-relieving devices like air mattresses or cushions.
-
Promote Healing:
- Maintain proper nutrition, emphasizing protein, vitamins (A, C), and zinc.
- Keep the wound moist and the surrounding skin dry.
-
Monitor Progress:
- Regularly assess wound size, depth, and signs of healing or complications.
- Change dressings as instructed, typically every 1-3 days or when soiled.
When to Seek Medical Help:
- The wound worsens or does not improve despite care.
- Signs of systemic infection (fever, chills, increased pain, or confusion).
- Extensive necrosis or worsening of the surrounding skin.
Would you like detailed instructions on advanced care techniques, dressing recommendations for a specific stage, or caregiver training for managing bedsores?
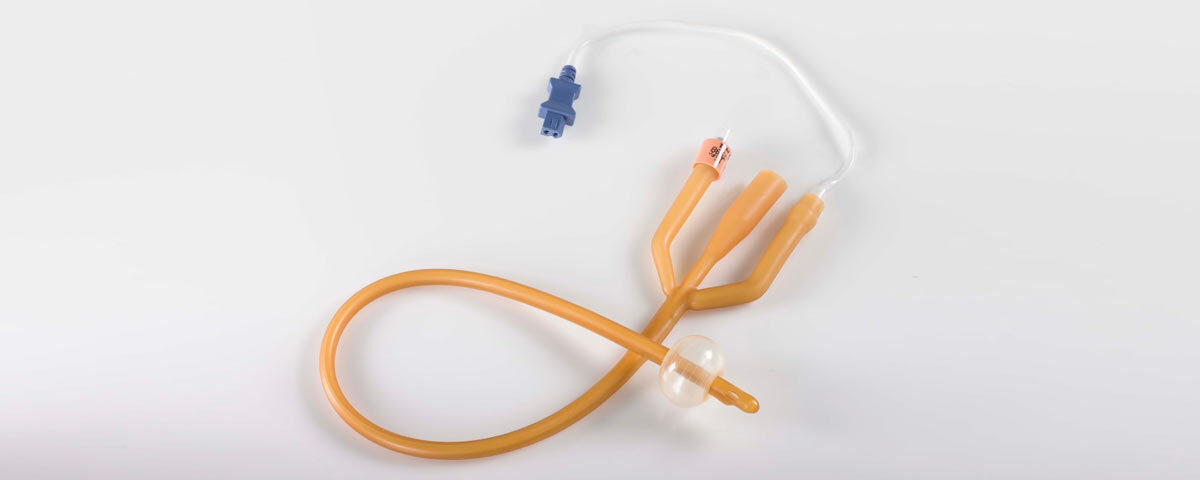
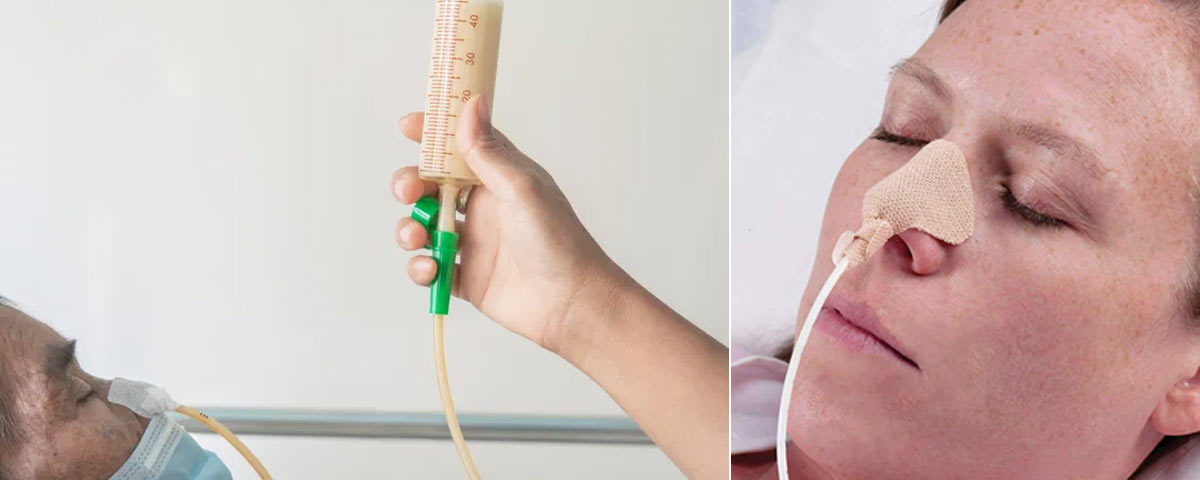
FOLEY’S CATHETERIZATION
Foley’s Catheterization is the insertion of a Foley catheter—a flexible tube passed through the urethra into the bladder—to drain urine. It is commonly used for patients who are unable to urinate naturally due to medical conditions, surgeries, or prolonged immobilization. Proper technique and aftercare are crucial to prevent complications such as infections or trauma.
Indications for Foley’s Catheterization:
- Urinary Retention: Inability to pass urine due to obstruction, neurological conditions, or post-surgery.
- Monitoring Urine Output: Especially in critical care settings.
- Urinary Incontinence: When other methods of management are not suitable.
- Surgical Procedures: During and after surgeries involving the bladder, prostate, or adjacent areas.
- Bladder Irrigation: To manage clots or prevent obstruction.
Equipment Required:
- Foley catheter of appropriate size (measured in French, e.g., 12–16F for adults).
- Sterile gloves and drape.
- Antiseptic solution (e.g., povidone-iodine or chlorhexidine).
- Sterile lubricant or anaesthetic gel.
- Catheter drainage bag.
- 10 mL sterile water for balloon inflation.
- Syringe for balloon inflation.
- Cotton balls or gauze.
- Disposable underpad.
- Securement device (e.g., catheter strap).
Steps for Foley’s Catheterization:
-
Preparation:
- Explain the Procedure:
- Inform the patient about the process and gain consent.
- Position the Patient:
- Males: Supine with legs slightly apart.
- Females: Supine with knees flexed and legs apart, exposing the perineal area.
- Ensure Privacy and Asepsis:
- Use a sterile drape and maintain a sterile field throughout the procedure.
-
Hand Hygiene and Gloving:
- Wash hands thoroughly and wear sterile gloves.
-
Cleansing the Urethral Opening:
- For males: Retract the foreskin (if uncircumcised) and clean the glans in a circular motion, starting from the urethral opening outward.
- For females: Separate the labia and clean from front to back using antiseptic-soaked gauze or cotton balls.
-
Insertion of Catheter:
- Apply Lubricant:
- Generously lubricate the tip and length of the catheter to minimize discomfort.
- Insert the Catheter:
- Gently insert the catheter into the urethral opening:
- Males: Advance the catheter to the bifurcation (where the balloon port is).
- Females: Advance the catheter until urine flows, then another 2-3 cm to ensure correct placement.
- Check for Urine Flow:
- Once urine flows, confirm the catheter is in the bladder.
- Gently insert the catheter into the urethral opening:
-
Balloon Inflation:
- Inflate the catheter balloon with sterile water (usually 5-10 mL, depending on the catheter size).
- Gently tug the catheter to ensure the balloon is properly seated against the bladder neck.
-
Connect the Drainage Bag:
- Attach the catheter to a closed drainage system.
- Secure the catheter to the patient’s thigh to prevent tension or displacement.
-
Final Steps:
- Dispose of used materials properly.
- Record the procedure, including the catheter size, amount of water used for inflation, and any observations.
Post-Procedure Care:
-
Ensure Hygiene:
- Clean the catheter insertion site daily with mild soap and water.
- Avoid harsh chemicals or excessive cleaning that can irritate the skin.
-
Monitor Output:
- Record urine color, consistency, and volume regularly.
- Ensure the drainage bag remains below bladder level to prevent backflow.
-
Prevent Infections:
- Do not disconnect the drainage bag unnecessarily.
- Replace the catheter as per medical guidelines or if signs of infection occur.
-
Secure Properly:
- Ensure the catheter is anchored to prevent movement and reduce the risk of urethral trauma.
Complications and Management:
-
Urinary Tract Infections (UTIs):
- Symptoms: Fever, cloudy urine, foul odour, or discomfort.
- Management: Notify the healthcare provider; antibiotics may be required.
-
Urethral Trauma:
- Symptoms: Pain, bleeding, or resistance during insertion.
- Management: Stop the procedure, assess, and seek expert help.
-
Catheter Blockage:
- Symptoms: Reduced or absent urine flow.
- Management: Flush the catheter with saline (if prescribed) or replace it.
-
Leakage Around Catheter:
- Cause: Bladder spasms or incorrect balloon inflation.
- Management: Reassess placement and balloon inflation volume.
Removal of Foley’s Catheter:
- Deflate the balloon completely using a syringe.
- Gently withdraw the catheter while observing for resistance.
- Monitor for urinary retention or discomfort after removal.
Would you like further guidance on training staff for Foley catheterization, managing specific complications, or selecting catheter sizes for different patients?